'Half our Covid patients are under 43': How the third wave has left a Paris hospital struggling to cope
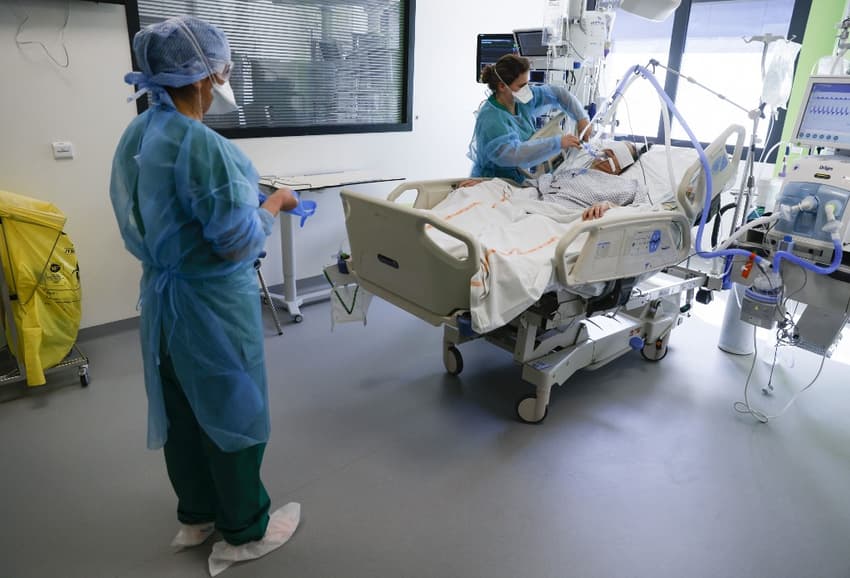
As Covid-19 rips through the impoverished Paris suburb of Seine-Saint-Denis, doctors are struggling to find beds for critical patients and teachers are walking out over a spike in infections in schools.
At the Delafontaine hospital, in the heart of mainland France's poorest region, the ravages of France's third wave of coronavirus infections are plain to see.
A 30-year-old man, who had no prior medical condition before being struck down by Covid-19, wakes up after three weeks in intensive care.
"This one has to get better," one nurse says to an orderly. "But I've learned not to have too much hope," she adds, after a moment's reflection.
As the number of critically ill patients across France soars past 5,000 - more that at the height of the second wave last autumn - Delafontaine has had to add eight more beds in intensive care, taking the total to 26.
With doctors in the Paris region warning they will soon have to start deciding who to save, two patients have already been transferred from Delafontaine to other facilities.
Daniel Da Silva, the head of Delafontaine's intensive care unit, is hopeful he will never have to turn patients away.
But he is worried about the profile of people now presenting severe symptoms in an area of densely-inhabited high-rise housing estates with a large immigrant population.
Half of the hospital's Covid-19 patients are under 43 years of age, who are far down the waiting list for a vaccine being administered in descending order of age.
And in a first for the hospital since the pandemic began, pregnant women are winding up in intensive care.
"We had to intubate and carry out an emergency Caesarean on a young woman aged 23," Da Silva says, calling it "unprecedented".
Seine-Saint-Denis currently has the second-highest incidence rates of Covid-19 in France, with 783 per 100,000 people, more than twice the national average.
Last week, around 30 teachers at a high school in the town of Drancy walked off the job saying they were in "imminent danger" of falling prey to a pandemic that has killed 20 people among its students' families in a year.
On Wednesday evening President Emmanuel Macron, who has so far resisted imposing a third countrywide lockdown, will address the nation to announce further restrictions.
READ ALSO What can we expect from Macron's TV announcement
Da Silva says his biggest concern is how to keep his unit staffed, with more and more carers getting written off work for stress or anxiety.
"People are exhausted and the issue of post-traumatic stress from the first wave is far from being resolved," he said.
Alice Auroux, a nurse who said she had not had a proper holiday in a year, gave voice to the despair that many healthworkers have expressed in the face of the government's failure so far to impose a stay-at-home order.
"It feels as if we're not getting on top of it," she said.
Mathilde Azzi, a young doctor who has cancelled her holidays and doubled her shifts to remain on the frontline, expressed particular concern for non-Covid patients.
Like all hospitals in the Paris area, Delafontaine has been ordered to cut back surgery to make space for Covid patients.
"They (non-Covid patients) are the ones who will pay the price," Azzi said, noting a decline in the number of patients being admitted for heart attacks, a trend she believed was caused by people failing to see a doctor on time.
As France girds for a further curtailment of freedoms, Da Silva said he understood the toll on the economy and nation's psychological wellbeing under stay-at-home orders.
"But at the same time I see what we're dealing with here. One thing is certain - with lockdowns, we saved more lives than we can count."
Comments
See Also
At the Delafontaine hospital, in the heart of mainland France's poorest region, the ravages of France's third wave of coronavirus infections are plain to see.
A 30-year-old man, who had no prior medical condition before being struck down by Covid-19, wakes up after three weeks in intensive care.
"This one has to get better," one nurse says to an orderly. "But I've learned not to have too much hope," she adds, after a moment's reflection.
As the number of critically ill patients across France soars past 5,000 - more that at the height of the second wave last autumn - Delafontaine has had to add eight more beds in intensive care, taking the total to 26.
With doctors in the Paris region warning they will soon have to start deciding who to save, two patients have already been transferred from Delafontaine to other facilities.
Daniel Da Silva, the head of Delafontaine's intensive care unit, is hopeful he will never have to turn patients away.
But he is worried about the profile of people now presenting severe symptoms in an area of densely-inhabited high-rise housing estates with a large immigrant population.
Half of the hospital's Covid-19 patients are under 43 years of age, who are far down the waiting list for a vaccine being administered in descending order of age.
And in a first for the hospital since the pandemic began, pregnant women are winding up in intensive care.
"We had to intubate and carry out an emergency Caesarean on a young woman aged 23," Da Silva says, calling it "unprecedented".
Seine-Saint-Denis currently has the second-highest incidence rates of Covid-19 in France, with 783 per 100,000 people, more than twice the national average.
Last week, around 30 teachers at a high school in the town of Drancy walked off the job saying they were in "imminent danger" of falling prey to a pandemic that has killed 20 people among its students' families in a year.
On Wednesday evening President Emmanuel Macron, who has so far resisted imposing a third countrywide lockdown, will address the nation to announce further restrictions.
READ ALSO What can we expect from Macron's TV announcement
Da Silva says his biggest concern is how to keep his unit staffed, with more and more carers getting written off work for stress or anxiety.
"People are exhausted and the issue of post-traumatic stress from the first wave is far from being resolved," he said.
Alice Auroux, a nurse who said she had not had a proper holiday in a year, gave voice to the despair that many healthworkers have expressed in the face of the government's failure so far to impose a stay-at-home order.
"It feels as if we're not getting on top of it," she said.
Mathilde Azzi, a young doctor who has cancelled her holidays and doubled her shifts to remain on the frontline, expressed particular concern for non-Covid patients.
Like all hospitals in the Paris area, Delafontaine has been ordered to cut back surgery to make space for Covid patients.
"They (non-Covid patients) are the ones who will pay the price," Azzi said, noting a decline in the number of patients being admitted for heart attacks, a trend she believed was caused by people failing to see a doctor on time.
As France girds for a further curtailment of freedoms, Da Silva said he understood the toll on the economy and nation's psychological wellbeing under stay-at-home orders.
"But at the same time I see what we're dealing with here. One thing is certain - with lockdowns, we saved more lives than we can count."
Join the conversation in our comments section below. Share your own views and experience and if you have a question or suggestion for our journalists then email us at [email protected].
Please keep comments civil, constructive and on topic – and make sure to read our terms of use before getting involved.
Please log in here to leave a comment.